Director of the Community Affairs Board, Australian Computer Society
Principal, Xamax Consultancy Pty Ltd, Canberra
Visiting Fellow, Department of Computer Science, Australian National University
Version of September 1992
© Xamax Consultancy Pty Ltd, 1992
This paper was presented as the Keynote Address to a Seminar of the Australian Medical Informatics Association (AMIA), Perth - 24 October 1992
This document is at http://www.anu.edu.au/people/Roger.Clarke/DV/PaperHCN.html
The health care sector comprises an enormous range of individuals and organisations, with highly diverse political perspectives. They are custodians of highly sensitive data. The liveliness of health informatics has recently been further stimulated by the proposal for a Health Communications Network (HCN). The establishment of a common infrastructure for the industry could offer significant potential benefits for patient care and for health care resource management. The HCN project was initiated by government agencies through the conference of Commonwealth and State Ministers for Health. To date the discussions have not directly involved the health care professions, nor representatives of health care consumers, or privacy and civil liberties groups.
This paper outlines the proposal as it is presently understood, and identifies concerns, of both a political and a privacy nature. Two alternative network patterns are described, one centralist in philosophy and the other open and democratic. A vehicle is suggested whereby the network design can reflect, and be seen to reflect, the interests of all of the many stakeholders in the Australian health care sector. Health care professionals, health care consumers, and privacy interests must combine their energies, to ensure that the development of the HCN is not dominated by a narrowly representative group.
Health care in Australia is provided through a mix of private enterprise and governmentally controlled institutions. Political tension among the participants is inherent. The health care sector generates and uses a vast amount of data. That which relates to patient care is very sensitive from the viewpoint of confidentiality and privacy. Partly because modern treatment practices are expensive, and partly because the need for treatment is distributed unevenly over the population, health insurance is a necessary feature of the industry. In order to exercise control over health insurance claims, insurers (whether government bodies or private companies) require considerable detail about transactions, and the right to conduct audits. Efficiency in the use of health care resources demands monitoring of the diagnoses, procedures, prescriptions and practices at all of the nation's 45,000 health care locations. As a result of these needs, a great deal of both identified and statistical data is transmitted to locations remote from the point of treatment.
Because so much of the health, health insurance and health resource management data traffic identifies individuals, it is highly privacy-sensitive. The primary focus is on the concerns of the patient, but health care providers are also identified and therefore have a privacy interest as well. In addition, aggregated data may give rise to commercial confidentiality interests on the part of providers.
With advances in information technology (IT) have come improvements in a variety of aspects of health care. To date most of these improvements have been within individual locations. IT also has the capacity to facilitate the delivery of data to any location where it is needed, when it is needed, irrespective of where the data was collected and where it is stored (Clayton & Grossman 1991). The Federal Government, in conjunction with the State Governments, has set out to establish a framework within which this promise can be fulfilled. The title chosen for the initiative is the 'Health Communications Network' (HCN).
This paper commences by providing background to the HCN project and its objectives. It identifies two areas of serious concern: the impact on privacy, particularly of patients but also of providers; and the potential for the project to be used by governments to centralise information and power, constrain the freedom of care providers, and in effect nationalise the health care industry.
The paper then outlines two alternative network models which are significantly different in their philosophies and in their implications for the future structure of the health sector. The open, democratic model can achieve the potential benefits while ensuring that the risks to privacy and freedoms are managed. The final section proposes a mechanism whereby the interests of all stakeholders in the system can be taken into account, and seen to be taken into account.
The genesis of the HCN proposal can be traced back some years. For example, in early 1989, a 'Health Information Network' was mooted, under the auspices of a joint venture between IBM, Medibank Private and the AMA-owned Australasian Medical Publishing Company. The resulting company, Mednetwork Systems, is now delivering to primary health care providers a practice management package including a variety of communications capabilities, including links among practices, and between practices, their support services and health insurers.
The immediate origin of the present HCN proposal was the adoption by the Australian Health Minister's Conference (AHMC) in September 1991 of a proposal by NSW that "consideration be given to developing a national health information systems and technology strategy covering both in-hospital and community-based care" (AHMC 1991, p.1). A joint Commonwealth/State Working Group was established, to report to the next AHMC in early 1992 "on how a durable basis for health information management and exchange might be established" (p.1).
A Workshop was held in Sydney in December 1991 on the 'National Health Information Systems and Technology Strategy'. Some 45 people were in attendance, predominantly from government agencies and hospitals, although members of the Australian Hospitals Assocation, the Medical Records Association and the Royal College of Nursing attended, in a private capacity. The Workshop was sponsored by the management consultancy arm of Digital Equipment Corporation. A partner in KPMG Peat Marwick, Mr Phillip Wing, led the team developing the proposal.
Observations arising from this Workshop were (pp.4-6):
A working document, generally known by its short title, 'Compelling Case' (AHMC 1992a), was prepared for a meeting of a sub-committee of the AHMC in February 1992. Its general recommendations (although not all details in the report) were accepted by that group and brought forward to the AHMC in April. That meeting of the AHMC endorsed "the development of a detailed business case and implementation plan for the Health Communications Network and Agency for consideration at the next AHMC" (AHMC, 1992b, p.1).
The 'Compelling Case' made only fleeting mention of participation by non-government organisations in the proposed process (single-line references on pp. 27 and 114). When discussing 'risk management', the document indicated that lack of consensus among clinicians was of medium likelihood and medium impact and that the recommended approach to managing this risk was "align then educate". Lack of consensus among private health practitioners was considered high likelihood, but low impact, with the recommendation to "leave till later". Consultation with outside groups was similarly treated in cursory manner (pp. 42, 55). Involvement of the private sector in joint public and private investment was referred to, but a voice for representatives of the private sector in the formation of the strategy appeared not to be contemplated (p.28). All measures within the project were referred to as "State and Commonwealth initiatives". There was considerable stress on 'education', 'marketing' and 'setting of the agenda'.
The concept of the Health Communications Network (HCN) was likened to an electronic equivalent to the Australia Post service: "Australia Post is a public utility offering every person in Australia should they wish to use it, the means to communicate paper-based information in envelopes. Australia Post is not interested in what is in the envelopes, but it does have certain rules for using the service. For instance, sending prohibited substances in the mail is not allowed and payment for the service is required by using a stamp" (p.3). Similarly, "the HCN ... communications utility will be available to every health care provider, manager, planner and funder, if they choose to use it, and will be capable of transporting authorised information to everyone in the health care system" (p.4).
Tenders were called in May, closing on 5 June, for the drafting of a business plan for the HCNA. Mr John Scott of the Department of Health was quoted in the Medical Observer of 29 May - 11 June 1992, as saying that the agency was likely to function similarly to Austel, which is the federal government's telecommunications regulatory arm. The consultancy brief (AHMC 1992c) stated that the project team was to work closely with Commonwealth and State government officers, It included no requirement, however, that key stakeholders such as health care providers and consumers participate in the development of the HCNA model, nor that they be involved in the governance of the HCNA, nor even that they be involved in any way in the preparation of the business case. The tender was won by a consortium managed by KPMG Peat Marwick. An interim report was required for consideration at a meeting of the AHMC in October, with completion scheduled for December 1992.
An appropriately conceived and implemented HCN might offer the prospect of significant benefits in the effectiveness of patient care and the efficiency of health care resource management, although the manner in which the anticipated benefits would arise needs careful analysis. Depending on how it is conceived, the HCN could have very serious negative impacts on patient and provider privacy and on private health care practice. The following two sections discuss these two areas of concern.
Australia is a mixed-market economy. It gains its primary impetus by harnessing the energy of self-interest (or 'greed', as the Prime Minister more forthrightly calls it) through the competitive supply of goods and services. These activities are subjected to self-imposed and governmental regulatory mechanisms, to ensure that adequate standards of quality and fairness are achieved. In some markets, governments are directly involved in the supply of services, particularly where they consider that competitive processes are undesirable or ineffectual.
During the last few decades, most of the countries which were committed to central economic planning and management have moved towards the adoption of what were previously maligned as 'capitalist' principles. Governments throughout Australia are undergoing a period of commercialisation and outsourcing of services which they consider are capable of being made more efficient if directly subjected to market forces.
Health care has greater government involvement than most other sectors of Australian industry. The bulk of hospital services are provided by State government agencies, and the primary health insurance service is an agency of the Federal government. The Federal Government conducts a running battle with the medical profession, seeking to rein in the spiralling costs of health care, which it considers to be closely associated with doctors' high earnings levels and high income expectations.
Medical practitioners perceive a tendency within the Commonwealth Government toward the centralisation of activities, and reduction in the freedoms enjoyed by private health care practitioners. Such a tendency is of course contrary to the trends evident elsewhere in the world, and in most other sectors in Australia.
From the perspective of medical consumers, there is evidence that the already high level of paternalism on the parts of both governments and health care providers is increasing. Medical science is becoming more sophisticated and remote, and less understandable. The influence of patients is low, the information available to them is limited, their scope for self-determination is low, and their choices are constrained variously by the medical professions, health care organisations, and health insurance provisions.
Public service employees are charged with the responsibilities of administering public funds, ensuring equity in the distribution and use of resources, and encouraging effectiveness and efficiency in health care. There is a 'sharp end' to these responsibilities: audit activities are necessary, to keep excesses, waste and private practitioner self-interest in check, and prevent, discover and prosecute fraudulent behaviour. In gathering the statistics they need to monitor resource usage and service levels, they doubt the capability and the trustworthiness of some participants, and accordingly seek access not only to aggregate data, but also to data about individual procedures.
In Australia, as in other advanced nations, a great deal is contributed toward the quality of products and services by the self-regulatory mechanism of formal standards. Standards Australia (SA) is a self-funding body which brings together diverse interests within particular industries, and operates consensually to establish requirements. Through Committee IT/14 and its Sub-Committees, SA has been active since early 1991 in establishing National Standards relating to the security of patient clinical data, and has published Draft Australian Standards relating to data held in organisations' records and in patient-held cards (SA 1992). The great strength of the Standards Australia approach is that the organisation itself has no vested interest in the shape of the outcome; it is a neutral party which provides a meeting venue for all industry participants, a publishing house and a distribution channel for those publications.
One of the roles proposed for HCNA is "to provide an umbrella for establishing and promulgating national standards and guidelines for health care communications" (AHMC 1992b, p.7). It thus appears that HCNA is to usurp Standards Australia's role. It would be most undesirable to replace established democratic processes by a Commonwealth/State government joint venture with little or no representation by industry participants, health care consumers or any other interested parties.
Although it would clearly be premature for anyone to cast judgement on the specific features of the HCN scheme, some aspects are already apparent. One which gives rise to concerns is the question of compulsory versus voluntary use by health care providers. It is disingenuous to suggest, as AHMC (1992a) does, that there will be freedom to use or not use the HCN. To extend the analogy used in the that document, Australia Post has a legislated monopoly, at least for the small items which make up the majority of the traffic. Apart from the economy of scale issues, the regulatory aims could not be achieved if the undisciplined and the criminal among the provider community could stay outside the scheme. It is accordingly difficult to believe other than that it would quickly become compulsory for all participants in the health care industry to be connected to the HCN, and receive and send messages using it. This makes broad participation in the scheme's conception and design all the more critical.
There are clear centralist tendencies both in the manner in which the HCN/HCNA proposals are being developed, and in some of the features of the proposal which is emerging. This exacerbates the fears already felt among many private health care practitioners that the Commonwealth government seeks progressive nationalisation of health care services, rather than a balance between private sector service provision and government control mechanisms.
The Commonwealth and State government agencies which have initiated the project control the vast majority of funds which flow in the health sector. They are therefore in a position to pursue their presumed aims. Other participants are distrustful of the government agencies involved, their motivations and their power. The HCN proposal is therefore at risk of meeting opposition from many of the participants whose cooperation is important if the scheme is to deliver its potential benefits. It is in the interests of all parties to overcome the climate of suspicion which is beginning to envelop the project.
Information privacy is a relatively recent preoccupation. A former Health Minister went so far as to denigrate is as a 'bourgeois value'. Until the last few decades, it was not necessary for people to express concern about it, or for Parliaments to create laws protecting it. This was because of the highly dispersed nature of data storage, the difficulty of finding data when it was wanted, and the difficulty of copying and transmitting the data once it was found; in other words, information privacy was protected by the enormous inefficiency of data handling.
Information technology has progressively reduced that inefficiency, to the great benefit of industry, commerce and government, and also of health care. Concomitant with those efficiency improvements, however, has been the disappearance of the traditional information privacy protections. New mechanisms are needed to ensure that society's headlong rush for efficiency does not mortally wound other critically important human values.
Privacy issues loom large in medical records systems, even where they operate within the boundaries of a single health care organisation. This is especially acute in organisations in which specialised health care is commonly provided to the same patient by multiple professionals, and in organisations which support or control front-line providers, and therefore handle data once-removed from the person to whom it relates. Combinations of technological and organisational measures are needed to ensure collection, processing, storage, access and disclosure practices are appropriately privacy-sensitive.
In a facility like the HCN, whose express purpose is to make data widely available, across organisational boundaries, across time, and across space, the privacy risks are an order of magnitude greater than those which arise in systems internal to a single medical practice, hospital, audit agency or insurer. The documentation so far available on the HCN makes several references to patient information privacy. In one of those references, privacy is identified as a cost, and it is argued that compliance costs of designing privacy requirements into the HCN will be lower than would be the case if they need to be grafted onto existing systems: "meeting privacy, confidentiality and security requirements for personal information in the health care system is becoming an increasingly significant cost issue ... The HCN provides the vehicle for a planned response to privacy, and therefore an opportunity to significantly reduce the costs of compliance" (AHMC 1992b, p.6-7).
Such spurious arguments are all too common in justification documents emanating from the Commonwealth public service. The simple facts are that most existing systems will need to have privacy-compliance grafted onto them in the coming years whether or not an HCN is implemented, and that the costs of designing privacy-enabling features into the HCN will be necessary additional costs, not alternative costs.
The proposal's more substantive discussion of privacy, confidentiality and security states that "privacy will be safeguarded, as it is now, at the individual site of collection ... Specifically, patient information will be held on the doctor's own system and will not be accessible by unauthorised people ... Transferring personal information ... will require appropriate doctor and patient approval ... the caller will have the ability to select the level of security required for the transmission" (AHMC 1992b, p.8-9). The last 20 years of promises about privacy features of new government systems have been mostly broken rather than honoured. Not only privacy advocates, but also many participants in the health care industry, will accept such statements only if a mechanism exists whereby they cease to be mere politicians' assurances, and become embedded in the conception of the project.
An aspect of the consultancy brief which gives rise to particular concern is that privacy is to be governed by "relevant privacy legislation". The Commonwealth Privacy Act 1988 has significant shortcomings, and requires enhancement to deal with any vast, new scheme such as the HCN. It applies, moreover, to only a fraction of the individuals and organisations involved in the Australian health care sector. Not one State presently has privacy legislation which complies with Australia's commitment to the OECD's 1980 Privacy Guidelines. Unless and until the HCN proposal embodies the creation of State laws protecting patient and provider information privacy, any assurance that the scheme complies with "relevant privacy legislation" is almost entirely empty.
A further factor, which has attracted particular attention among some commentators, is the possibility that a chip-card may be used as a means of patient identification and/or patient data-storage. In any information system, whether manual, supported by standalone computers, or supported by a integrated, nationwide network, data subjects need to be identified. This may be done on an informal basis (depending on the knowledge and judgement of the person dealing directly with the patient), using things which the patient knows (such as a membership number, their birthdate or their mother's maiden name or birthsign), something that the patient has (e.g. a token such as magnetic-stripe or chip-card, with or without a number and/or a photograph on it), or something that the patient is (e.g. their fingerprint, their DNA, or, to take efficiency to extremes, an implanted chip or brand).
There are various advantages and disadvantages in each possible identification mechanism. A chip-card differs from other tokens, in that it has significant storage capacity and possibly also significant intrinsic processing power. There are many different ways in which that storage and processing power can be used. How it is used determines the extent to which a scheme would infringe, or indeed protect, the information privacy of patients and health care providers. It is therefore pointless to either laud or attack any suggestion as to the use of chip-cards unless and until the nature of the proposed use is clarified.
As regards the risks to the information privacy of health care providers, the documents available to date appear not to mention it at any point. Given the intention to use the network for the transmission of health care resource management data, and the instances which have arisen in which some agencies have inadequately protected such data, provider privacy would appear to be an important topic, worthy of early treatment.
Information privacy risks are implicit in any system which provides efficient data management and communication. The nature and extent of the risks involved will be different, however, depending on the philosophy underlying the scheme's design, and the particular features designed into it. My own judgement, as both an information technologist and a privacy advocate, is that acceptable levels of freedom for health care professionals and information privacy for patients and providers can be achieved in an HCN. This is borne out by the work of health informaticians who are developing privacy-sensitive prototype systems (e.g. Nugawela 1991, Andrews & Wilkins 1992).
The next section examines two alternative network patterns which could be adopted in the development of the HCN, and argues that the open, democratic model is more protective of both freedoms and privacy, possibly no less effective and efficient, and certainly more robust and adaptable than the centralised form.
A detailed description of computer networking would necessarily involve highly technical language. Fortunately such a deep understanding is not essential to enable a discussion of the appropriate general form for the HCN. It is sufficient to focus on the layout, or 'topology', of networks.
A network comprises 'nodes' which are computers, and 'arcs' which are links between computers. Nodes may be of many different shapes and sizes (of varying processing power, data-storage and data-access capabilities, etc.), and so can arcs (which vary in such particulars as the volume of data they can transmit in a given time - their 'bandwidth'). Where two nodes are not directly connected to one another, they communicate via a 'path' comprising a series of arcs and nodes.
A 'network topology' is a pattern of connections among nodes. Two which are relatively easily described (although seldom used) are the 'daisy-chain', in which all of the nodes are strung along a single path, like a set of Christmas tree lights; and a 'fully-interconnected' network, in which every node is connected to every other node. A fully-interconnected network is extremely expensive, and a daisy-chain is extremely fragile.
Any network is subject to disturbances. In order to achieve high levels of reliability (i.e. to ensure that services are seldom unavailable due to failures of nodes or arcs) and robustness (i.e. to provide quick recovery after services have been interrupted), it is necessary to design redundancy into the system. This takes the form of multiple nodes offering the same service and access to the same data, and multiple paths connecting any given pair of nodes.
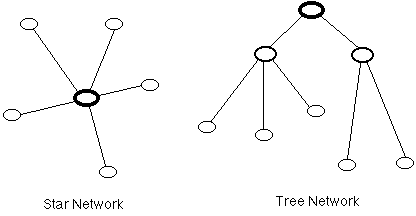
Many different topologies are possible. This paper considers two distinct families. One approach involves recognising one node as being central to the network, and making all other nodes subservient to it, in what is commonly referred to as a 'star network'. This idea may be refined further, such that intermediate nodes have intermediate levels of rights, and a 'tree' structure is established. Such networks, depicted in Exhibit 1, can be described as having a 'hierarchical' topology.
A hierarchical topology is appropriate in a context in which notions such as 'authority' and 'centralisation' are important. Decisions are made at relatively few, superordinate nodes. Information flows from subordinate nodes, which specialise in data-collection, towards superordinate nodes, which are oriented towards decision-making.
Systems of this kind exist, and can function very satisfactorily in some contexts. Apart from computer-based applications such as industrial control systems, the human neural system can be explained using this model. In principle, a military command and control system ought to have a hierarchical topology. In practice, however, a military system generally functions in a hostile environment, and centralised networks are fragile. They can function with the highest degree of effectiveness and efficiency, but only while narrowly defined conditions hold. Their robustness under pressure, and their adaptability to changed circumstances, are very limited, such that their effectiveness and efficiency decline catastrophically when real-world complexity gets the better of them.

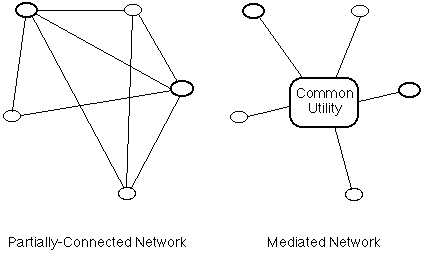
Another, quite different, approach to networks is to identify nodes as being 'peers' with equal authority, or with comparable degrees of authority, but in respect of different functions; for example, each node may take responsibility for all processing and storage relating to a particular aspect of the system's functionality (e.g. support of a particular regional clinic, or epidemiological research into a particular class of diseases), and have special rights recognised by all other nodes in that regard (say the right to access, respectively, to identified data relating to particular patients, and to re-identifiable data relating to nominated diseases and procedures). Similarly, particular kinds of data held at each node (say data identifying a patient) may be recognised as being controlled by that node and require special authority before it can be released to any other node. Two alternative forms such an 'open topology' network can take are shown in Exhibit 2.
An open topology is consistent with the processes of a free society, in which protected enclaves (like the home) are respected, until and unless, via due process, a condition is demonstrated under which an enclave can be justifiably invaded in fulfilment of some higher interest. Open topology networks are appropriate in contexts in which nodes are specialised as to their function and/or geographic scope (such as scores of differently specialised classes of service-centre, mapped across 45,000 locations scattered over the largest island in the world), and/or where network robustness and adaptability are important.
The two network models discussed in this section are, intentionally, extremes. In practice, any realistic alternative would incorporate elements of both concepts. The purpose of presenting the extremes has been to establish that the Health Computing Network could be conceived to serve any philosophy ranging from totalitarian to highly devolved. The more the HCN resembles the centralised model, the greater the threats to freedoms and privacy; whereas the more it reflects the open, democratic model, the greater the extent to which freedoms and privacy can be sustained, consistent with at least satisfactory levels of effectiveness and efficiency, and probably superior levels of robustness and adaptability.
The next section addresses the question as to what type of vehicle is necessary in order to ensure that the conception, design, development and maintenance of the HCN will use the open, democratic model.
The HCN proposal originated from a meeting of Health Ministers. That is in no way to be criticised, but rather to be applauded, as reflecting the kind of strategic thinking citizens expect from their Governments. In its present form, the proposal is for a Health Communications Network Agency (HCNA) to be established. This "may be a Commonwealth/State joint venture and could operate as a private company. Its roles would be to negotiate with carriers ... for communications capacity ..., provide an umbrella for establishing and promulgating national standards and guidelines ..., and provide platform for future technology and information systems investments" (AHMC 1992b, p.7).
The initiative was developed from suggestions by a small group of individuals attending a workshop in a private capacity, and is a creation of Commonwealth and to a lesser extent State government agencies. Organisations other than government agencies have had no influence to date, even though the finalisation of a business plan for the undertaking is imminent.
It is, of course, possible that a government agency might act in a manner reflecting the needs of all stakeholders, and produce as fair an outcome as any more complicated procedure would achieve. Few of the parties concerned, however, would be likely to express confidence in that happening. A participative process is needed in any case, such that the many relevant representative organisations affected by the proposal can understand the idea, influence it, 'bond with' it, and commit themselves and their members to it. In the words of a Canadian report: "the co-ordination/co-operation which is essential ... can only be based on consensus through authoritative compromise among equal persons who represent all health constituencies" (Wilk, 1991, p.3).
As a result of the proposal's genesis within the confines of government agencies, there is a real risk that many interested parties will be suspicious of, and even automatically opposed to, the HCN project. Such an attitude would probably be to the detriment of health care in Australia. Rather than committing themselves to an adversarial stance, health care providers, health care consumers and privacy and civil liberties interests must bring forward constructive proposals for a mechanism whereby the HCN can be opened out into a collaborative project. This is akin to the notion of a 'research partnership' among the interested parties (NCEPH, 1991).
The argument in this paper leads to two specific suggestions. The first relates to the constitution and governance of the HCNA. It should be an organisation quite distinct from the Commonwealth and State Governments, and from the agencies directly involved in its creation. At least two alternative models could be used. One is that which on which the Australian Meat and Livestock Corporation (AMLC) is based. This is formed under an Act of the Federal Parliament, but represents the interests of the pastoral industries' participants, and manages a network which supports on-line trading in livestock. An example of the other model is Tradegate, which is a company formed under the Companies Act and owned by the international trade community, which provides a forum for all stakeholders in that industry (including those which are not shareholders), and which has commissioned a network services supplier to provide networking services for members of that community. Whatever model is chosen, it is clear that agencies of the Commonwealth and State governments must be recognised as stakeholders within the health care industry and the HCNA, not only as external regulators.
The second suggestion relates to the mechanism whereby models for the HCNA and the HCN should be formulated. In an industry as large, complex and politicised as health care, it is not appropriate for Governments to impose solutions, but rather to bring the parties together, and to exercise ultimate, but delicate, control. A forum is needed, at least in the short term, whereby the stakeholders can meet, discuss the objectives, canvass the issues, consider alternative models, and reach consensus upon the constitution and governance for the HCNA and the nature of the HCN.
To again use Canadian words: "A Health Information Co-ordinating Council (HICC) should be established (via grassroots consultation and nomination) which is acceptably representative of all health constituencies - government (health ministries and other) and non-government (for profit and not-for-profit)" (Wilk 1991, p.4, emphasis in original). Only by a multilateral cooperative process can the necessary mutual confidence be developed that the Health Communications Network will be a shared resource, rather than a means whereby one set of players will be able to dominate the others.
The HCN promises much to Australians. Depending on how it is conceived, designed and implemented, it may also threaten much that is valuable to Australians.
It is imperative that the scheme's design, and the philosophy underlying it, be subjected to critical consideration, negotiated over and approved by a body representing all affected parties.
To achieve that end, health care professionals, health care consumers and privacy and civil liberties groups must urge the creation and empowerment of a suitably constituted vehicle to drive the HCN project. The Governments and government agencies which have initiated the project must adjust from the hitherto closed procedures to open mechanisms directly involving all constituencies .
I was stimulated to address this topic as a result of a series of conversations with Patrick Nugawela, President of the Australian Medical Informatics Association (AMIA) and Chair of the Australian Computer Society's Health Care Committee.
Important information was provided to me not only by Patrick, but also by Dallas Ariotti of the Commonwealth Department of Health, Housing & Community Services, Dick Thrussell of Standards Australia, and Stephen Milgate and Simon Davies of the Australian Doctors' Fund. Needless to say, the interpretations, judgements, arguments and conclusions in the paper are not attributable to any of these people, but are mine alone.
AHMC (1991) 'Report on the National Health Information Systems and Technology Strategy Workshop - December 16-18 1991' (37 pp., un-numbered). Available from the Hospitals Branch, Dept of Health, Housing and Community Services, Canberra
AHMC (1992a) 'Compelling Case: Report of the Joint Federal/State Steering Committee for Health Information Management and Technology' (February 1992) (140 pp.). All but Appendix F - Overall Project Plan, pp. 64-83, available from the Hospitals Branch, Dept of Health, Housing and Community Services, Canberra
AHMC (1992b) 'A National Health Information Systems and Technology Strategy' Report of the AHMC Working Party to the Aust. Health Ministers' Conference (14 April 1992) (11pp.). Available from Hospitals Branch, Dept of Health, Housing and Community Services
AHMC (1992c) 'Consultancy Brief for a Health Communications Network and Agency Business Case' AHMC Joint Commonwealth/State Working Party for Health Information Management and Technology (May 1992) (7 pp.) Available from the Hospitals Branch, Dept of Health, Housing and Community Services
Andrews G. & Wilkins G.E.J. (1992) 'Privacy and the Computerised Medical Record' The Med. J. of Aust. 157 (Aug 17, 1992) 223-225
Clayton P.D. & Grossman D.D. (1991) 'Current Developments and Future Trends in Information Technology in Health Care' Proc. Conf. Trends in Modern Hospital Information Systems, Göttingen, Germany (Sep 1991)
NCEPH (1991) 'Health Information Issues in General Practice in Australia' Discussion Paper No. 2, National Centre for Epidemiology and Population Health, Australian National University, 1991
Nugawela P. (1991) 'AMIA-Net: A Pilot Project to Link Medical Practitioners With Various Instrumentalities, Service Providers and Professional Institutions' Aust. Medical Informatics Assn, Perth (Feb 1991)
SA (1992) 'Standards in Health Informatics'. 'Patient-Held Medical Record Cards' and 'Security of Patient Clinical Data in Electronic Clinical Information Systems' Draft Australian Standards 92123-5, Standards Australia, 15 July 1992
Wilk M.B. (1991) 'Health Information for Canada: Report of the National Task Force on Health Information' National Health Information Council, Ottowa (1991)
Go to Roger's Home Page.
Go to the contents-page for this segment.
Last Amended: 13 October 1995
 | These community service pages are a joint offering of the Australian National University (which provides the infrastructure), and Roger Clarke (who provides the content). |  |
| The Australian National University Visiting Fellow, Faculty of Engineering and Information Technology, Information Sciences Building Room 211 | Xamax
Consultancy Pty Ltd, ACN: 002 360 456 78 Sidaway St Chapman ACT 2611 AUSTRALIA Tel: +61 2 6288 1472, 6288 6916 |